Plantar hyperhidrosis, also known as sweaty feet, is a common disorder characterized by excessive sweating on the soles of the feet. The condition is a subtype of hyperhidrosis in areas with a high density of eccrine sweat glands, like the feet. As the primary type of hyperhidrosis, however, plantar hyperhidrosis typically results in excessive sweating of the feet while awake, independent of environmental conditions. It usually causes extreme foot odor, fungal infections, and slippery feet, making it hard for the affected individual to wear specific footwear like high-heeled shoes and sandals.
Sweaty feet appear early in life, usually showing between ages 0 to 11. The condition results not from having increased sweat glands but from idiopathic hyperactivity of the eccrine sweat glands, the sweat glands responsible for homeostasis and thermoregulation.
Although a few studies showed that it is more prevalent among females than males, more is needed to fully assert the gender-based incidence of sweaty feet. Sweaty feet also reportedly affect approximately 5 percent of the entire global population, though the exact figures are unknown as some people find it embarrassing to admit to having sweaty feet. What is clear, however, is that the condition stems from different causes, most of which are listed below.
Overactive Thyroid
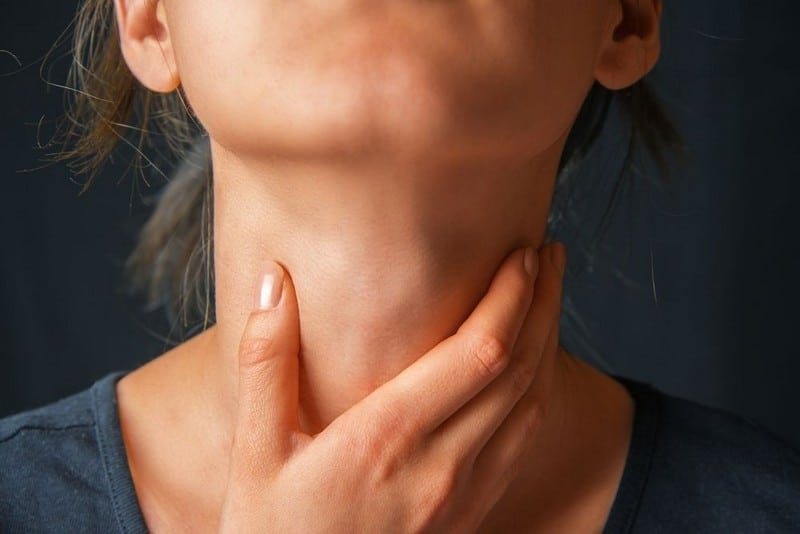
Hyperthyroidism, or overactive thyroid, is a condition that occurs when the thyroid, a butterfly-shaped gland at the base of the neck, produces too much of one of the main thyroid hormones, thyroxine. The release of too much thyroxin in the bloodstream can cause hyperthyroidism. It affects the person’s energy level, weight, metabolism, heart rate, bowels, mood, cholesterol levels, bones, menstrual cycles (among women), and sensitivity to heat.
Hyperthyroidism and its symptoms, particularly the one that makes an individual extremely sensitive to heat, usually results in excessive sweating, characterized by plantar hyperhidrosis or sweaty feet. It also causes severe weight and body fat loss as the body struggles to adjust to and compensate for the hormonal imbalance.
Though extremely rare, hyperthyroidism isn’t exactly incurable. With the help of a medical practitioner, people with hyperthyroidism can be diagnosed through either a physical exam of the neck, blood tests, or imaging tests like radioactive iodine uptake (RAIU) test, thyroid scan, or thyroid ultrasound. Treatment plans usually vary, from the use of antithyroid drugs like methimazole (Tapazole) to propylthiouracil (PTU), oral intake of radioactive iodine, beta-blockers, or surgical removal of the thyroid gland (thyroidectomy).